|
|
||||
|
Monday, November 13, 2023
|
|
||||
|
||||
|
||||
|
||||
|
||||
|
||||
|
||||
|
| Stay connected with Government Executive: | ||||
|
| GOVERNMENT EXECUTIVE // CONTACT US // PRIVACY POLICY // UNSUBSCRIBE |
|



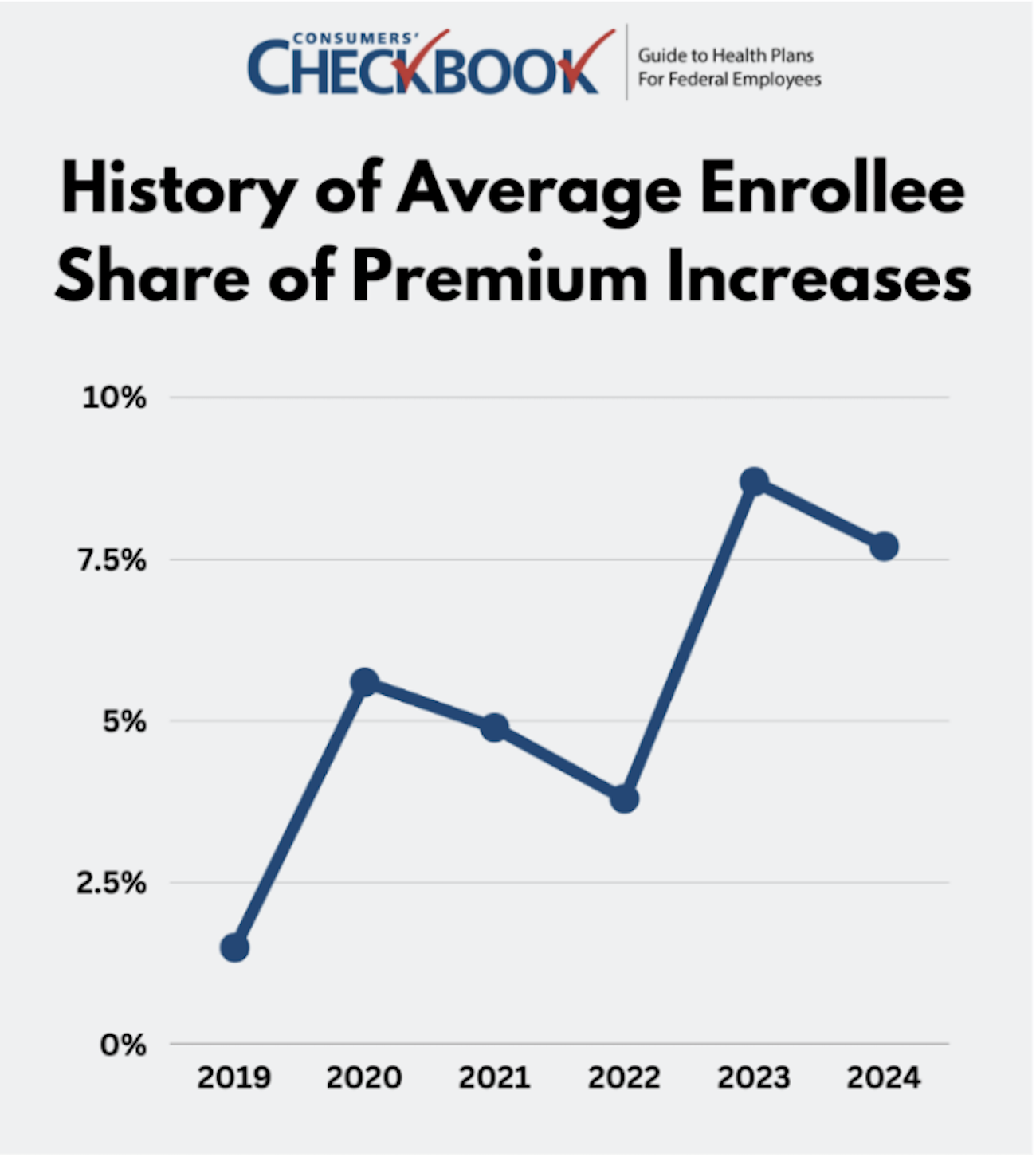 Next years 7.7% premium increase is less than the 8.7% increase of 2023, but it's still much higher than previous years. In 2022, the average enrollee increase was only 3.8%. While no one can predict the future, federal employees and annuitants should prepare to pay higher premiums and a higher rate of increase going forward.
Next years 7.7% premium increase is less than the 8.7% increase of 2023, but it's still much higher than previous years. In 2022, the average enrollee increase was only 3.8%. While no one can predict the future, federal employees and annuitants should prepare to pay higher premiums and a higher rate of increase going forward.  Some of the changes are striking. For example, the largest decrease in enrollee share of premium is from the Baylor Scott & White Standard Health Plan (A8), available in Central Texas, which costs 54% less in 2024, saving self-only enrollees around $1,500 next year. Aetna Advantage, a national PPO plan, has the same premium in 2024 as 2023. The largest increase in enrollee share of premium is from Kaiser Permanente High (F8) in the Atlanta region, which is 22% more in 2024 and will cost self-only enrollees around $1,100 more next year.
Some of the changes are striking. For example, the largest decrease in enrollee share of premium is from the Baylor Scott & White Standard Health Plan (A8), available in Central Texas, which costs 54% less in 2024, saving self-only enrollees around $1,500 next year. Aetna Advantage, a national PPO plan, has the same premium in 2024 as 2023. The largest increase in enrollee share of premium is from Kaiser Permanente High (F8) in the Atlanta region, which is 22% more in 2024 and will cost self-only enrollees around $1,100 more next year.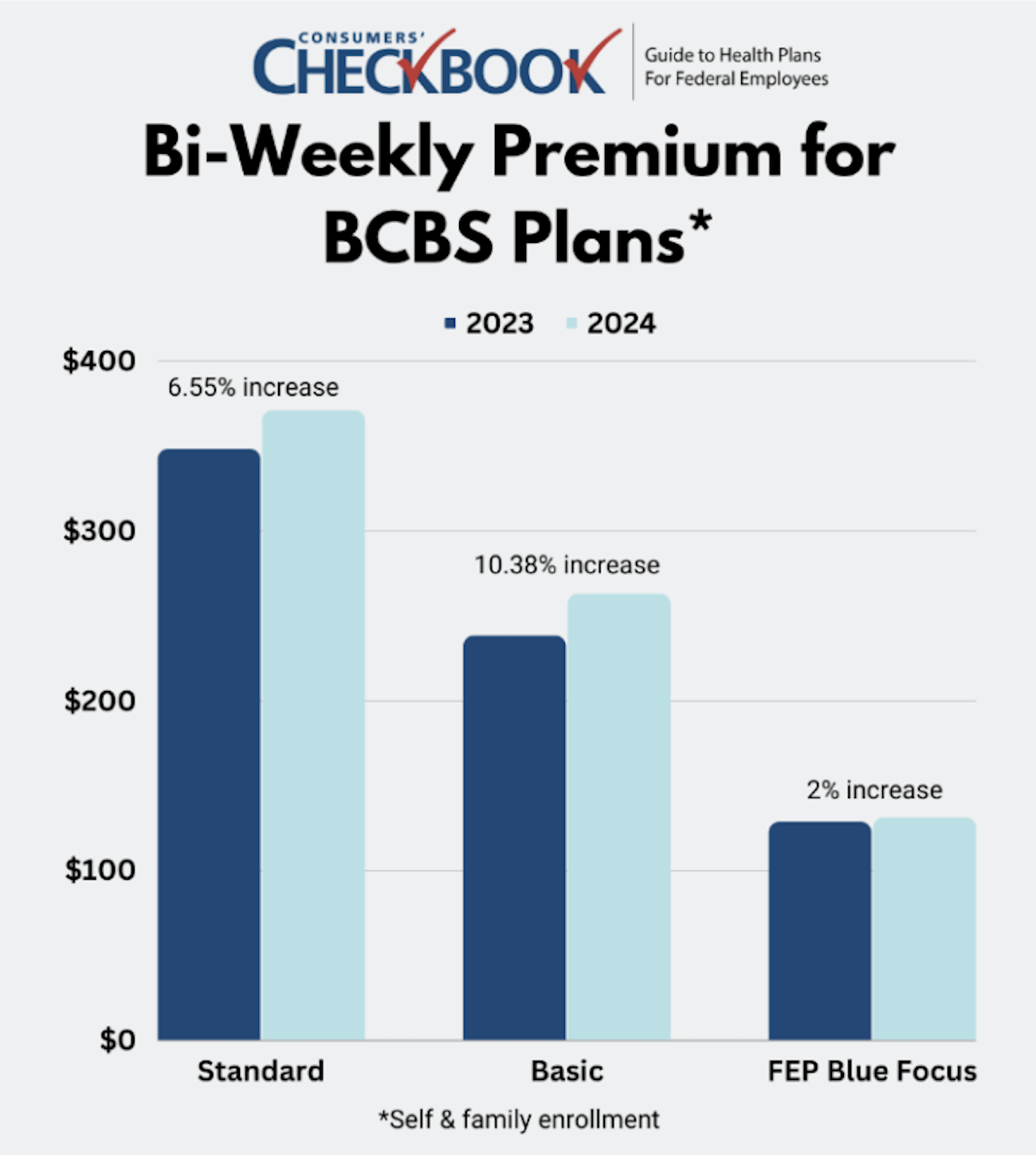 This upcoming Open Season is a good opportunity to assess whether your current plan is still the best fit for your needs. For Basic and Standard plan members, are you enrolled in the right BCBS plan? Now might be the opportunity for you to save one or two thousand dollars a year in premium by switching to FEP Blue Focus.
This upcoming Open Season is a good opportunity to assess whether your current plan is still the best fit for your needs. For Basic and Standard plan members, are you enrolled in the right BCBS plan? Now might be the opportunity for you to save one or two thousand dollars a year in premium by switching to FEP Blue Focus. 